Acute and Rehab Hospitals May Be Viable Under Medicare Cuts
The Issue You Tackled
The Affordable Care Act (ACA) mandates Medicare payment growth rate reductions to acute and rehab hospitals and home health providers. CMS/OACT initially calculated that these reductions would cause most such providers to become unprofitable by 2040, likely leading to widespread hospital closures and adverse impacts for patients. But this calculation was simplified and ignored several dynamic factors.
What You Actually Did
During 2012-2014, we developed an SD model that addressed the dynamic factors. One of them was population aging, which along with increased insurance coverage under the ACA, may help boost provider profits by increasing volumes and revenues.
If profits still decline, then provider reactions, such as downward adjustments in their breadth or availability of services, would help providers protect themselves in terms of costs, but at the same time may hurt patients and lead to more hospital readmissions and even deaths.
The model was tested with respect to multiple uncertainties and simulates several outcome metrics of importance to taxpayers, patients, providers, and communities.
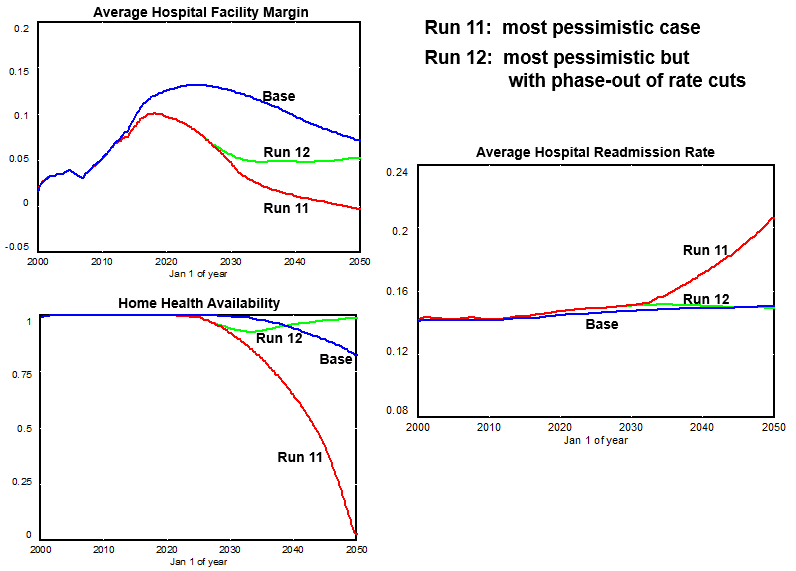
The Results
Most acute and rehab hospitals will likely maintain healthy profit margins in the coming decades despite the Medicare cuts and without the need for service cutbacks–due to the aging population, ACA insurance expansion, and the ability of most hospitals to reasonably handle somewhat higher bed occupancies than they have today. But home health agencies will not fare as well, and some will close. A worst-case scenario could start to hurt hospitals by the 2030s; but in this case the rate cuts could be phased out, and the system could be stabilized.
| Name | How Medicare Payment Rate Reductions Will Affect Hospitals and Patients |
|---|---|
| Modelers | Jack Homer, Gary Hirsch |
| Client/Participant | Centers for Medicare and Medicaid Services, Office of the Actuary (CMS/OACT) |
| Client Type | Government |
INFORMS Annual Meeting
This case was presented at the INFORMS Annual Meeting in November of 2014 in San Francisco, California. Please find the slides that were used during the presentation here.
OTHER SUCCESSFUL APPLICATIONS
Solving Bottlenecks in Dairy Production Facilities with System Dynamics
Solving Bottlenecks in Dairy Production Facilities with System Dynamics EXECUTIVE Summary FrieslandCampina faced potential bottlenecks in production due to the merging of two factories. They hired SD&Co which employed system dynamics simulation models to predict...
A Design Value Calculator: A System Dynamics Boardgame
A Design Value Calculator: A System Dynamics Boardgame EXECUTIVE Summary Product design is a specific form of complex innovation that touches all areas of an organization’s management. While entrepreneurs recognise the value of design, they often tend to focus...
The World Bank Uses System Dynamics to Identify Root Causes of Poverty
The World Bank Uses System Dynamics to Identify Root Causes of Poverty EXECUTIVE Summary Madagascar has one of the highest poverty rates in the world. In 2022, an astonishingly three out of every four people in Madagascar lived below the poverty line. Poverty has...
Upcoming Events

MIT System Dynamics Seminar | Approaches to Encouraging Health Exchange Participation
You are invited to attend the System Dynamics Seminar being held on Friday, April 26th from 12:30-2:00pm EST in the Jay W. Forrester conference room, E62-450, or via Zoom: https://mit.zoom.us/j/94114971874 (Password: SDSP24). Our guest speaker will be Soheil Ghili...
Recent Posts
Society Governance Updates
Society Governance Updates Welcome, Allyson! New President Allyson Beall King joined the Policy Council as our 2024 President. Her primary role is as director of the Washington State University School of the Environment, which focuses on regional ecologies and our...
Call for Presenters: Seminar Series
Call for Presenters: Seminar Series We at the System Dynamics Society are continually seeking vibrant and knowledgeable presenters for our ongoing Seminar Series. As we unfold the calendar, there’s always a place for more insights, experiences, and expertise to enrich...
Honoring Excellence: A Glimpse into the Awards of the International System Dynamics Conference
Honoring Excellence: A Glimpse into the Awards of the International System Dynamics Conference The International System Dynamics Conference brings together experts, practitioners, and students to exchange ideas, showcase real-world applications, and celebrate...
Join us
OTHER SUCCESSFUL APPLICATIONS
Solving Bottlenecks in Dairy Production Facilities with System Dynamics
Solving Bottlenecks in Dairy Production Facilities with System Dynamics EXECUTIVE Summary FrieslandCampina faced potential bottlenecks in production due to the merging of two factories. They hired SD&Co which employed system dynamics simulation models to predict...
A Design Value Calculator: A System Dynamics Boardgame
A Design Value Calculator: A System Dynamics Boardgame EXECUTIVE Summary Product design is a specific form of complex innovation that touches all areas of an organization’s management. While entrepreneurs recognise the value of design, they often tend to focus...
The World Bank Uses System Dynamics to Identify Root Causes of Poverty
The World Bank Uses System Dynamics to Identify Root Causes of Poverty EXECUTIVE Summary Madagascar has one of the highest poverty rates in the world. In 2022, an astonishingly three out of every four people in Madagascar lived below the poverty line. Poverty has...
Recent Posts
Society Governance Updates
Society Governance Updates Welcome, Allyson! New President Allyson Beall King joined the Policy Council as our 2024 President. Her primary role is as director of the Washington State University School of the Environment, which focuses on regional ecologies and our...
Call for Presenters: Seminar Series
Call for Presenters: Seminar Series We at the System Dynamics Society are continually seeking vibrant and knowledgeable presenters for our ongoing Seminar Series. As we unfold the calendar, there’s always a place for more insights, experiences, and expertise to enrich...
Honoring Excellence: A Glimpse into the Awards of the International System Dynamics Conference
Honoring Excellence: A Glimpse into the Awards of the International System Dynamics Conference The International System Dynamics Conference brings together experts, practitioners, and students to exchange ideas, showcase real-world applications, and celebrate...
Upcoming Events

MIT System Dynamics Seminar | Approaches to Encouraging Health Exchange Participation
You are invited to attend the System Dynamics Seminar being held on Friday, April 26th from 12:30-2:00pm EST in the Jay W. Forrester conference room, E62-450, or via Zoom: https://mit.zoom.us/j/94114971874 (Password: SDSP24). Our guest speaker will be Soheil Ghili...



