System Dynamics Helps Reduce Waiting Lines for NHS Patients
System Dynamics Real-World Examples and Case Studies
Need Help With a Complex Problem?
Looking for a Systems Consultant? Fill out this form and we will follow up with a call and, soon enough, the right person for the job. Meet our Executive Director, Rebecca Niles, to swiftly identify how to meet your needs. We can introduce Systems Thinking to your organization through renowned exercises like the Beer Game.
Nov 2021
by Vanessa Perez Perez
EXECUTIVE Summary
The impact of COVID-19 on the National Health Service (NHS) in England, led to growing record waiting lists, deterioration of patients and recovery of elective care became the number one priority.
Creative solutions were needed to tackle the elective recovery backlog, however, the health service in Norfolk and Waveney in the East of England were constrained by limited resources. System Dynamics allowed operational and clinical staff to test the impact of major interventions, aiding decisions for leaders in the system about where best to allocate resources and transform services to benefit patients and reduce waiting times.
The modelling exercise explored ways to address backlogs in the Musculoskeletal pathway with the aim of returning them to sustainable levels while providing good outcomes for patients. The insights provided by the model considered not only capacity restrictions but also the final outcomes for patients.
The model starts from the population and incidence of activity, and through the community (including GP referrals, diagnostics, community physiotherapy), before then moving through into secondary care. Moving into secondary care it covers first appointment, follow up, waiting lists, beds, and incorporates how trauma impacts on elective waiting lists while considering constraints in theatres capacity and community services.
#England #NHS #Health #Waiting lists #Musculoskeletal
The Problem
Integrated care systems (ICSs) are partnerships of organisations that come together to plan and deliver joined up health and care services, and to improve the lives of people who live and work in their area. Norfolk and Waveney Integrated Care System (ICS) in England had a number of challenges across the health system which comprises three acute hospitals, two community providers, and a mental health trust. Prior to COVID-19, elective care across Norfolk and Waveney ICS was already seeing increases in waiting lists and it was not meeting national standards with some patients waiting over 52 weeks for planned care. COVID-19 then saw the postponement of the elective care which further impacted the situation negatively, leading to one of the biggest cohorts of 104 week waits in England.
To tackle the challenges across the whole system, clinical and non-clinical colleagues came together with the support of NHS England and Whole Systems Partnership, to develop three System Dynamics models in Stella Architect starting with the Trauma and Orthopaedics speciality within the Musculoskeletal (MSK) pathway and then also models for the Dermatology and Eye Care pathways. The models were used to test different scenarios and identify how healthcare operational interventions designed to reduce the elective care backlog impact patients across the Norfolk & Waveney ICS system.
The Solution
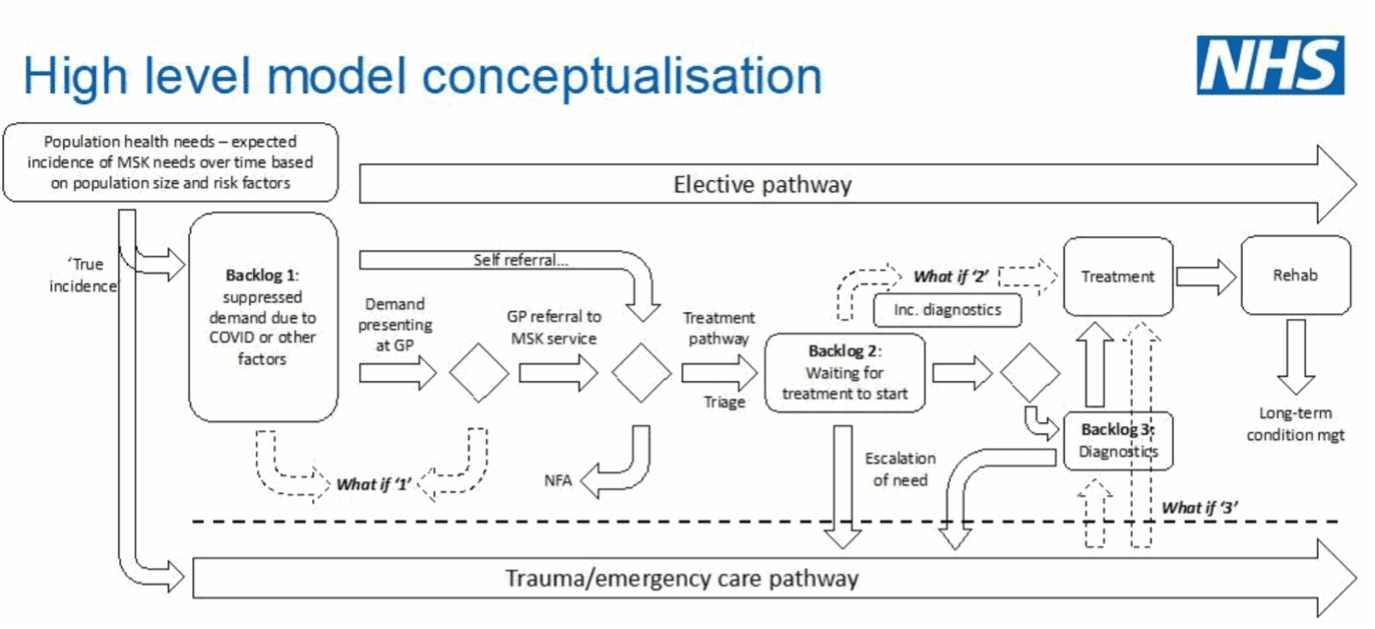
For the MSK pathway model, a group of analysts across the system first engaged with clinical and operational colleagues in stakeholder workshops identifying the key issue, exploring what-if questions, and developing a high-level conceptualisation of the model.
The model was developed using a modular approach by building separate parts of it first and then bringing the various components together. A user interface was created to support operational colleagues to understand the outputs of the model and enable decision-making. Operational colleagues used the interface to interactively adjust variables such as expected demand and see impact projections on capacity and waiting lists.
The model was able to test the following ‘what if’ scenarios:
What if…
…we provided open access to early self-referral and self-management including advice on holistic/lifestyle choices to improve ultimate outcomes and minimize the impact of delays caused directly or indirectly by the COVID epidemic?
…we deployed a multi-disciplinary team Advanced Clinical Practitioners (ACP) to triage long-wait patients and fast track those in greatest need, possibly to other providers, facilitating this with integrated IT systems?
…we eliminated interruptions to the capacity and therefore flow along the elective pathway from trauma or unscheduled care requirements, i.e. protected capacity?
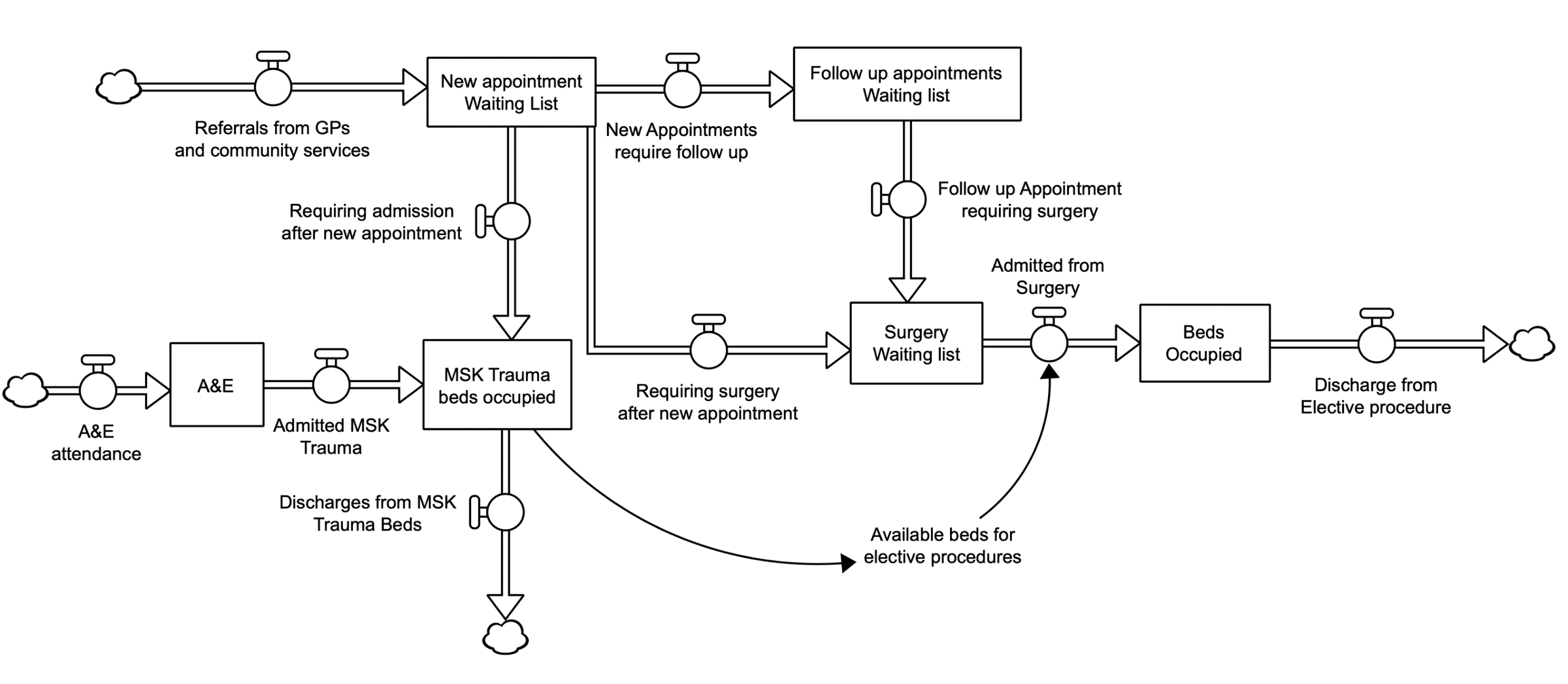
Once the high level model conceptualisation was agreed upon, a prototype model was developed by analysts across the system, who had begun to receive technical training in using the software. Analysts from across the system each took a different part of the system to model and once these were completed, the different parts were brought together to create the complete system model. The stock and flow diagram below shows main components in the model. Please note that the actual model is more complex than the one illustrated in the diagram.
The user interface was accessible through a link on the internet, which allowed password holders to use and run the model.
Outcomes
There were many significant benefits and impact for doing this work including enabling high quality operational decision making around the elective recovery. This work helped to develop cohesion within the ICS, improving working relationships between analysts, clinicians, and operational staff across all of the stakeholders in the region.
Here are some highlighted benefits and impact of creating a system model in Norfolk and Waveney:
> Different impacts of scenarios could be understood and visualised through the model
> End users are now testing their own what-if questions, and understanding how changes to parts of the pathway will impact other parts of the system
> An iterative process captured a multiplicity of voices with real life experiences of the service
> This project complemented existing quality improvement and elective recovery work happening in Norfolk and Waveney ICS
> Staff shifted from silo working to genuine system working
> More conversations are now happening about the harmonisations or pathways, the locations of diagnostic assessment centres and community hubs.
> This approach is empowering discussions with Integrated Care Boards at a system level
> Analysts are now equipped with technical skills in order to conduct system modelling
> Analysts have developed much closer relationships with clinicians.
learn more
Model
Please note that this is an example model, it is not validated and it does not contain genuine data – it should be used to understand what the tool looks like and should not be used operationally.
Connect with Vanessa Perez Perez
OTHER SUCCESSFUL APPLICATIONS
Solving Bottlenecks in Dairy Production Facilities with System Dynamics
Solving Bottlenecks in Dairy Production Facilities with System Dynamics EXECUTIVE Summary FrieslandCampina faced potential bottlenecks in production due to the merging of two factories. They hired SD&Co which employed system dynamics simulation models to predict...
A Design Value Calculator: A System Dynamics Boardgame
A Design Value Calculator: A System Dynamics Boardgame EXECUTIVE Summary Product design is a specific form of complex innovation that touches all areas of an organization’s management. While entrepreneurs recognise the value of design, they often tend to focus...
The World Bank Uses System Dynamics to Identify Root Causes of Poverty
The World Bank Uses System Dynamics to Identify Root Causes of Poverty EXECUTIVE Summary Madagascar has one of the highest poverty rates in the world. In 2022, an astonishingly three out of every four people in Madagascar lived below the poverty line. Poverty has...
Recent Posts
Society Governance Updates
Society Governance Updates Welcome, Allyson! New President Allyson Beall King joined the Policy Council as our 2024 President. Her primary role is as director of the Washington State University School of the Environment, which focuses on regional ecologies and our...
Call for Presenters: Seminar Series
Call for Presenters: Seminar Series We at the System Dynamics Society are continually seeking vibrant and knowledgeable presenters for our ongoing Seminar Series. As we unfold the calendar, there’s always a place for more insights, experiences, and expertise to enrich...
Honoring Excellence: A Glimpse into the Awards of the International System Dynamics Conference
Honoring Excellence: A Glimpse into the Awards of the International System Dynamics Conference The International System Dynamics Conference brings together experts, practitioners, and students to exchange ideas, showcase real-world applications, and celebrate...
Upcoming Events

MINDS Cast Ep. 4 – Systems Thinking Application in International Development w/ Amitaksha Nag
May 7 at 10 am NY | 3 pm London | 10 pm Beijing | Time Converter In this webinar, Amitaksha will share his insights about application of systems thinking in development projects and policy making. He will focus on conceptualizing systems-level (feedback,...

